by Ivan | Apr 2, 2019 | Medications, Patient News

Smoking Out the Myths: Medical Marijuana
Does medical marijuana offer a solution to treating epilepsy, chronic pain, anxiety and neurogenerative diseases? Or is it an untested, potentially unsafe treatment that will eventually turn out to be more of a pipe dream? As with so many of today’s biggest questions, the truth is somewhere in between. We bring you a down-to-earth view of this much-discussed and yet oft-misunderstood topic to separate the hype from the hope and dispel some Medical Marijuana Myths.
While the marijuana or hemp plant has been used for more than 3,000 years, research and treatment today is primarily focused on the extract known as CBD, a cannabinoid. Unlike one of the other chemicals in the plant, THC (tetrahydrocannabinol,) CBD has no psychogenic effects and does not produce the “high” commonly associated with marijuana. Hundreds of CBD-related tests are now in progress, and CBD products are available at dispensaries, online and are making their way into everything from coffee and yogurt to pet treats.
Last June, a major milestone was reached when the U.S. Food and Drug Administration (FDA) approved the CBD drug Epidiolex for two rare, severe forms of treatment-resistant epilepsy. Epidiolex, along with dronabinol and nabilone (which are synthetic cannabinoids previously approved to treat nausea from chemotherapy that has not responded to standard therapy), are now the only FDA-approved cannabis-based drugs.
The FDA was careful to note about Epidiolex: “This approval serves as a reminder that advancing sound development programs that properly evaluate active ingredients contained in marijuana can lead to important medical therapies. Controlled clinical trials testing the safety and efficacy of a drug, along with careful review through the FDA’s drug approval process, is the most appropriate way to bring marijuana-derived treatments to patients. Because of the adequate and well-controlled clinical studies that supported this approval, prescribers can have confidence in the drug’s uniform strength and consistent delivery.”
High hopes
The FDA’s cautionary tone was necessary because of the many well-publicized clinical and preclinical trials underway to test marijuana and its extracts. Interest continues to grow, as evidenced by the numerous research projects in progress. The most prominent studies are focused on chronic pain, trying to evaluate whether marijuana is a safer and less addictive alternative to opioids.Other research is aimed at testing if cannabinoids improve the symptoms of multiple sclerosis, Alzheimer’s disease, Parkinson’s disease, anxiety and insomnia, as well as its potential role in anti-inflammatoryand antiviral activity, blocking cell growth and preventing the growth of blood vessels that supply tumors.1
As promising as the research appears, it’s important to realize that at this time, not enough large, clinical trials have been conducted to show that the benefits of marijuana outweigh the potential risks. Research is still preliminary and much remains unknown about CBD and other cannabinoids’ optimal dosing range and the best route of administration (by mouth, inhaled, topically or sprayed under the tongue). Importantly, because they are not FDA-approved, the levels of THC or CBD can differ greatly from one dispensary to another or one batch to another.
Side effects are also hard to predict because potential impurities and variations in dosage are not addressed as they are in all FDA-regulated products. We are only starting to evaluate side effects which may range from minor dry mouth and dizziness, to death. It is also unclear if the products interact with other medications. An added concern is that older and sicker people may be more vulnerable to the drug’s side effects.
Our bottom line: although CBD is readily obtainable in most parts of the United States, and laws legalizing its use for medicinal purposes continue to pass, we need to take a step back and realize the process is far from complete. The fact is the scientific evidence does not yet support many of the claims to ease symptoms of certain diseases, improve quality of life and relieve pain, nor has it been approved for use as a cancer treatment. As Cleveland Clinic’s head of Employee Health Services recently pointed out, medical marijuana has not yet undergone extensive clinical trials, public hearings and approval by the FDA, or been thoroughly tested for safety and efficacy. His recommendation is one we can all support – focus on research that isolates specific compounds found in marijuana, produces a dose-specific medication, and submit it to testing and regulatory processes.
1 National Cancer Institute, 2019
Did You Know?
330
Number of cannabinoid research projects supported by the National Institutes of Health in 2017
34
Number of states (including the District of Columbia) that have approved the medical use of cannabis as of 2018
The post Medical Marijuana Myths appeared first on Specialdocs Consultants.
by Ivan | Apr 2, 2019 | Medical Conditions, Patient News

Attention Please: ADD/ADHD is Not Just a Childhood Condition
In the 21stcentury, it’s standard procedure to test unfocused, impulsive and restless children who struggle to achieve in school for Attention Deficit Disorder (ADD) and Attention Deficit Hyperactivity Disorder (ADHD), and provide support and treatment well into adulthood. But for those who came of age prior to the 1970s, that diagnosis was rarely made, leading to a lifetime of challenges. Only now, as ADHD and ADD are recognized as conditions that often do not disappear with maturity, are some seniors finally finding the answer to problems that have haunted them for years in Adult ADD.
ADD is a condition of varying degrees, and in cases of milder severity, whether in the young or older patient, can be difficult to diagnose; especially in older adults, because the symptoms are different than in children. Hyperactivity is rarely the primary indicator, although remnants are felt such as restlessness and talking too much. Most frequently experienced by adults is a tendency to be easily distracted, a decline in working memory and a lack of focused attention. As we get older, the challenge may lie in distinguishing these issues from the normal aging process, mild cognitive impairment or early dementia. Forgetting names, misplacing things, or having problems with organization and planning can be hallmark traits of ADD or an aging brain. The key to identifying the difference is longevity of symptoms. ADD doesn’t suddenly appear full-blown in an adult, but leaves a years-long trail of distraction in its wake.
What are Symptoms of Adult ADD?
Experts advise that symptoms can shift with age, but these are found fairly consistently in older adults with ADD*:
- “Swiss cheese memory,” characterized by things that slip through the cracks
- Issues with working memory, such as being easily thrown off course mid-task
- Misplacing items
- Forgetting words or names, brain going ‘blank’ periodically
- Difficulty learning new things
- Talking excessively, often without realizing it
- Interrupting others
- Trouble following conversations
- Difficulty maintaining relationships and keeping in touch
According to the organization ADDitude, a leading source of information, support and advocacy for people living with ADHD, asking this simple question – “Would you have been talking about these symptoms 20 years ago?” – can be one of the most accurate of all indicators. Patients who answer in the affirmative, remembering constantly being chided for a messy room, branded as a daydreamer or underachiever, and finding it difficult to keep organized and on time at a first job, are more likely to have previously undiagnosed ADHD. In fact, the majority would say “I can’t remember a time that I wasn’t this way.”
Gratifyingly, adults who are diagnosed with ADHD or ADD in their older years find it can be revelatory to finally identify the cause of their ongoing challenges, and receive the support they need at a particularly vulnerable life stage. Coping with ADD as a senior actually parallels the issues faced by young people with ADHD when they leave home. The loss of structure for both groups can strain their ability to adequately care for themselves, and poor sleeping or eating habits can result, which exacerbate ADHD symptoms. However, treatment which may include appropriate doses of stimulant medication and cognitive behavioral therapy, has been shown to work as well for adults as children, and provide a newfound satisfaction with life.
As Dr. David W. Goodman, assistant professor of psychiatry and behavioral sciences at the Johns Hopkins University School of Medicine and director of the Adult Attention Deficit Disorder Center of Maryland, explains: “People may ask, ‘if you’ve had this problem for so long, why bother treating it now?’ Imagine you believed yourself to be as others labeled you throughout your life – careless, irrational, a daydreamer, dumb or just plain odd. Then, you realize a treatable disorder caused these symptoms, and they aren’t a reflection of who you are. It’s liberating to understand the difference between what you have – a disorder – and who you are – a person.”
*Source: Kathleen Nadeau, Ph.D. presentation at the 2018 Annual Meeting of the American Professional Society of ADHD and Related Disorders
Did You Know?
Although ADHD and ADD is a commonly seen psychiatric condition in the US, second only to generalized depression, adults in their 50s, 60s and 70s often go undiagnosed and untreated.
Fewer than half of adults with ADHD ages 45+ have ever sought any kind of treatment and only 25% have tried medication.
Source: www.additudemag.com
The post Adult ADD appeared first on Specialdocs Consultants.
by Ivan | Jan 11, 2019 | Medical Conditions, Patient News

Higher Anxiety? Our ‘age of anxiety’ began four centuries ago
It can come on suddenly and intensely, causing shaking, confusion and difficulty breathing for no apparent reason…trigger an irrational avoidance of elevators or public transportation…or become a steady drumbeat of worry always in the background. All are known as anxiety disorders, one of the country’s most commonly experienced yet largely untreated mental health issues. Is our era of 24/7 disturbing news, packed schedules and often unrealistic expectations spurring a rise in these disorders, or does it just seem that way? Are we in the midst of the Age of Anxiety?
Modern life can be disquieting, but the truth is that anxiety disorders have always impacted large numbers of people around the world. Consider this description of Hippocrates’ patient in 1621’s The Anatomy of Melancholy: “He dare not come into company for fear he should be misused, disgraced, overshoot himself in gestures or speeches, or be sick; he thinks every man observeth him” – a classic case of what would now be diagnosed as social anxiety disorder. Recent research notes that anxiety disorders may be under-recognized and under-treated, but there is no evidence that its prevalence has increased. While the incidence rose from 9 to 15 percent in college students since 2009, according to the Journal of American College Health, the authors attribute the finding to a greater willingness to admit having a mental health issue and increased acceptance of it as a bona fide health problem.
Constant anxiety undeniably takes a toll on health, potentially increasing levels of the stress hormone cortisol and raising blood pressure and may drive inflammation and plaque formation that leads to heart attack and strokes. A reaction to stress that occurs in a region of the brain called the amygdala, anxiety prepares people to confront a crisis by putting the body on alert. The ‘fight or flight’ response serves us well when faced with actual danger but is counter-productive when dealing with worries around work, money, family life or health. However, it’s only when daily function is affected that a disorder is diagnosed, as shown below:
Everyday Anxiety: Worry about finances, health, family or other important life issues
Anxiety Disorder: Constant and unsubstantiated worry that causes significant distress and interferes with daily life
Everyday Anxiety: Embarrassment or self-consciousness in an uncomfortable or awkward social situation
Anxiety Disorder: Avoiding social situations for fear of being judged, embarrassed or humiliated
Everyday Anxiety: A case of nerves or sweating before a big test, business presentation, stage performance or other significant event
Anxiety Disorder: Seemingly out-of-the-blue panic attacks and preoccupation with the fear of having another one
Everyday Anxiety: Realistic fear of a dangerous object, place or situation
Anxiety Disorder: lrrational fear or avoidance of an object, place or situation that poses little or no threat of danger
Everyday Anxiety: Anxiety, sadness or difficulty sleeping immediately after a traumatic event
Anxiety Disorder: Recurring nightmares, flashbacks or emotional numbing related to a traumatic event that occurred several months or years before
The American Psychology Association defines these types of anxiety disorders (obsessive-compulsive disorder and post-traumatic stress disorder are now categorized separately):
- Generalized anxiety disorder (GAD): the most common, it’s characterized by excessive, long-lasting worries about nonspecific life events, objects and situations.
- Panic disorder: brief or sudden attacks of intense terror and apprehension, leading to shaking, confusion, dizziness, nausea and breathing difficulties; can occur with or without a particular trigger.
- Specific phobia: irrational fear of a particular object or situation.
- Agoraphobia: fear of places, events, or situations, especially open spaces, that may cause you to panic and feel trapped, helpless or embarrassed.
- Social anxiety disorder: fear of negative judgment from others in social situations or of public embarrassment.
- Separation anxiety disorder: not exclusive to youngsters, but also experienced by adults who feel disconnected from a person or place that provides feelings of safety or security.
Additionally, anxiety disorders may play a role in exacerbating other conditions such as irritable bowel syndrome (IBS), chronic respiratory disease and heart disease.
Reassuringly, the number of treatment options, both pharmaceutical and non, has grown. Most effective is a combination approach of psychotherapy (cognitive-behavioral therapy, focused talk therapy or exposure therapy), stress management (deep breathing, meditation and yoga) and antidepressant and/or anti-anxiety medications.
Finally, considerable benefits are seen from a healthy lifestyle – reduced intake of caffeine, tea, cola and chocolate, avoidance of recreational drugs and excessive alcohol, and emphasizing exercise, a nutritious diet, and most importantly, a good night’s sleep. According to a recent University of California at Berkley study, the amygdala was particularly stimulated when sleep deprived, mirroring that of anxiety disorders, suggesting that sleep therapy could reduce anxiety in people suffering from panic attacks, GAD and other conditions.
Did You Know?
40 million
People in the U.S. affected by anxiety disorders
Source: NIMH.gov
37%
Percentage of Americans with an anxiety disorder who receive treatment
Source: ADAA.org
The post The Age of Anxiety appeared first on Specialdocs Consultants.
by Ivan | Jan 11, 2019 | Nutrition, Patient News
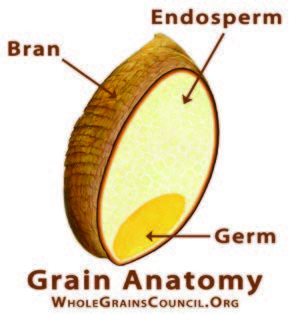
Going with the (Whole) Grain
Whole Grains may be the culinary trendsetters of the 21st century, but the ancient wonders of the grain world have remain unchanged for the last several hundred years. From chia to kamut, sorghum to spelt, like many whole grains, they are significant sources of protein, fiber and other important nutrients, such as B vitamins, iron, folate, selenium, potassium and magnesium.
You may already be familiar with quinoa, which became one of the first ancient grains to trend in U.S. kitchens earlier in the decade. You’ll find more below, each a story to tell and a taste to be discovered:
Amaranth,* native to Peru and a major food crop of the ancient Incas, has a peppery taste and a versatile cooking profile – bake it with bananas, use it to coat chicken or fish or toss with vegetables for a fresh salad.
Farro goes back 10,000 years to the time of the Fertile Crescent, and is thought to have sustained the Roman army. Key to Mediterranean diets, this grain is higher in dietary fiber than quinoa and brown rice and lower in calories. Its dense, chewy texture works well in soups, risottos and is thought by some aficionados to make the best pasta.
Freekeh, frequently found in Middle Eastern and North African cuisine, has roots in ancient Egypt. A form of wheat known for its chewy texture and nutty flavor, it’s often sold cracked into smaller, quicker cooking pieces. Use in pilafs and salads, or cook into a delicious porridge.
Kamut, also known as Pharaoh grain in a nod to its discovery in ancient Egyptian tombs, is rich and buttery-tasting, ideal in breads, pancakes and salads, or in a breakfast bowl with avocado and other whole grains, such as quinoa.
Millet,* a staple of the long-lived Himalayan Hunzas, is likely to be more familiar to Americans as a birdseed ingredient, but this grain has a delicious, nutty like flavor. Cook as a hot cereal, steam and use in salads or bake in breads and cookies.
Quinoa,* cultivated by the Inca in the Andes, has become even more popular on the American table in recent years. Dozens of varieties exist, from mild-flavored white and yellow to earthier tasting red and black. Prepare as a breakfast cereal, substitute it for rice and pasta, add to soups and salads, or pop and eat like popcorn.
Sorghum,* from Asia and West Africa, is a source of protein, and can be substituted for wheat in baked goods, eaten like popcorn or cooked into porridge.
Teff,* from Ethiopia and Eritrea, is a smaller-sized, quick-cooking grain high in iron and calcium, with a sweet molasses-like flavor that can be cooked into a polenta or ground into flour to make gluten-free breads and baked goods.
*Gluten-free
Sources: Harvard Health & Whole Grains Council
The post Whole Grain Superfood appeared first on Specialdocs Consultants.
by Ivan | Jan 11, 2019 | Industry Insights, Patient News, Wellness

Why Today’s Health News Often Becomes Tomorrow’s Retractions
We’ve all seen it played out hundreds of times, as a drug, food or habit is trumpeted as the way to lower the risk of cancer or heart disease only to be walked back the next month in another study. The reasons can be diverse, including a flawed hypothesis, bad data or misleading conclusions, but at the center is the study design itself. A longitudinal trial may yield very different findings from an observational one, while the gold standard – a randomized controlled trial (RCT) – can be extremely costly and difficult to design. The resulting patchwork of research requires professional analysis and a wait-and-see approach until confirmation is received via follow-up studies. We share some expert insights to help you view new health studies with both a healthy skepticism and the realization that some of the most important medical breakthroughs of recent years have been discovered in just this way.
Fast Facts on Health Studies
1,400
Number of scientific papers retracted each year
Sources: Vaccine Journal August 2018, Centers for Disease Control, Harvard Health
50%
Percentage of scientific studies confirmed in follow-up studies
Source: Healthy Aging Project, University of Colorado, Boulder
Researchers agree that a randomized, controlled trial is the best way to learn about the world. In a drug study, for instance, a population is randomly divided into groups who receive the drug and those who don’t. If properly controlled and designed, any difference in outcomes between the groups can be measured and credibly attributed to the effects of the treatment. The methodology is highly valued in evidence-based medicine, proving that associations are causal, and not just by chance. The approach has powerful real-world applications, as seen in the Women’s Health Initiative (WHI), one of the nation’s largest-ever health projects.
Begun in 1993, with more than 161,000 women enrolled, the randomized, controlled clinical trial was designed to test the efficacy of long-term hormone therapy in preventing heart disease, hip fractures and other diseases in post-menopausal women over 60 years old on average. Previous observational studies had strongly suggested the preventive benefits of hormone therapy, and it was routinely recommended for women years after menopause. What happened next was stunning.
In 2002, the trial was halted three years earlier than planned as evidence mounted that the estrogen plus progestin therapy significantly raised a woman’s chances of developing cardiovascular disease, stroke and breast cancer. Millions of women stopped taking hormone therapy, and the trial has since been credited with reducing the incidence of breast cancer by 15,000-20,000 cases each year since the results were made public. Numerous follow-up studies were conducted to dig deeper into the surprising data, and while they showed that hormone therapy may still be reasonable short-term to manage menopausal symptoms in younger women, it is no longer routinely recommended years after menopause to prevent chronic disease in women.
Similarly, Vitamin E supplements, once thought to reduce risk of heart disease, were found to not have beneficial properties and actually may increase the risk of heart disease in higher doses. Consequently, the American Heart Association now advises that the best source of Vitamin E is foods, not supplements.
The biggest takeaway from both initiatives: the critical need for randomized, controlled trials to prove that associations between an intervention and a disease are causally related.
Nutrition health studies have also come under increased scrutiny, especially with the recent revelation of erroneous data published by high-profile researcher Dr. Brian Wansink, founder of the Food and Brand Lab at Cornell University. Numerous papers have been retracted as the lab’s propensity for data dredging – running exhaustive analyses on data sets to cherry pick interesting and media-friendly findings – came to light. This practice, seen somewhat frequently in food and nutrition research, may be part of why contradictory headlines seem to be the norm.
As the adage goes, data can be tortured until it says what the researcher wants to hear. That’s why your physician will always be the best source for making sense of the tremendous amount of health data released each day…so please ask!
Testing by Design
The most commonly used research models include:
Randomized controlled trial (RCT): carefully planned experiments like the WHI that introduce a treatment or exposure to study its effect on real patients; includes methodologies that reduce the potential for bias and allow for comparison between intervention groups and control groups.
Observational studies: researchers observe the effect of a risk factor, diagnostic test, treatment or other intervention without trying to change who is or isn’t exposed to it. Includes cohort studies, which compare any group of people linked in some way (e.g. by birth year); and longitudinal studies in which data is gathered for the same subjects repeatedly over years or even decades. An example is the Framingham Heart Study, now in its third generation, which has provided most of our current consensus regarding the effects of diet, exercise and medications on heart disease.
Case control study: compares exposure of people with an existing health problem to a control group without the issue, seeking to identify factors or exposures associated with the illness. This is less reliable than RCTs or observational studies because causality is not proven by a statistical relationship.
Meta-analysis: a thorough examination of numerous valid studies on a topic, which uses statistical methodology to combine and report the results of multiple studies as one large study. This is cost-effective but not as accurate as RCTs as the individual studies were not designed identically.
The post Health Studies: Expert Insight appeared first on Specialdocs Consultants.
by Specialdocs Consultants, LLC | Sep 25, 2018 | Nutrition, Patient News

Finding the Path to Better Health Through Your Diet
In the quest for a healthier lifestyle, even inveterate beef eaters may be considering a more vegetable-centric diet. If you’re on a journey to vegetarianism or simply curious about the side roads surrounding it, follow our road map to nutritious eating and decoding diets with the expert direction of Jen Bruning, RDN, Academy of Nutrition and Dietetics.
What Kind of Eater are You?
Flexitarian is a term recently coined to describe those who eat a mostly vegetarian diet with occasional forays into meat. “Flexitarian is probably the most relatable, allowing people to take a stepwise approach to less meat,” says Bruning. “Instead of building a meal around beef, it becomes a side dish, ingredient, or is eliminated altogether.” The flexibility is key to real life applications. “If you’re at a barbecue you can enjoy without guilt.”
Dietary notes: No real challenges in terms of meeting dietary needs – follow the traditional healthy ‘plate’ but place more emphasis on vegetables, and substitute beans and legumes for meat when possible.
Pescatarian refers to those who abstain from eating all meat and animal flesh with the exception of fish. It’s becoming increasingly popular as a healthier way to eat or as a stepping stone to a fully vegetarian diet. “This can be a very balanced way of eating,” confirms Bruning, “as fish are rich in protein and Omega-3 fatty acids.” Some pescatarian diets include eggs and dairy.
Dietary notes: Avoid fish that contain higher amounts of mercury e.g. marlin, orange roughy, swordfish. Instead, opt for cod, tilapia, trout, canned light tuna, whitefish, salmon and sardines, among other choices.
Lacto-Ovo-Vegetarian is the more traditional vegetarian diet, eliminating beef, pork, poultry, fish, shellfish or animal flesh of any kind, but including eggs and dairy. It can be a nutritionally complete way of eating. Good sources of protein include legumes (lentils, beans, peas), soy-foods (tofu, tempeh, edamame), seitan, meat alternatives (veggie burgers, plant-based crumbles), milk, nuts, seeds, and grains (farro, millet, quinoa). Incorporate foods high in iron: dark leafy greens, beans, tofu, tempeh, black strap molasses, quinoa and tahini. Calcium requirements can be met with leafy green vegetables, tofu, and calcium-fortified products.
Dietary notes: Add vitamin C-rich food, such as tomatoes, bell peppers or citrus fruit, to increase iron absorption, such as beans in tomato sauce.
Vegans do not eat meat of any kind, or eggs, dairy products, honey or processed foods containing these or other animal-derived ingredients.
Dietary notes: To ensure adequate nutrition, incorporate the following foods or take a vitamin:
- Vitamin B12 – fortified foods
- Vitamin D – fortified orange juice or mushrooms treated with UV light
- Iron – dark leafy greens and Vitamin C-rich foods to help with absorption
- Calcium – kale and turnip greens
- Omega-3 fatty acids – flax seed, chia, walnuts
- Iodine – iodized salt or sea vegetables
Avoid the Raw Vegan/Raw Food diet, which is based on a nutritionally incorrect premise that cooking foods above 118 degrees F is harmful to the body.
The post Decoding Diets appeared first on Specialdocs Consultants.







Recent Comments